Lab Tests to Monitor Before Starting Once-Weekly Insulin
Thinking about starting a once-weekly insulin? That’s a big step, and like with any new medication, especially one that affects your blood sugar, it’s smart to get a good handle on what’s going on in your body first. Before you even think about that first shot, there are some important lab tests your doctor will likely want to run. These aren’t just random checks; they give us a baseline, a snapshot of your health right now, which is super important for figuring out the right plan and making sure the insulin works best for you. We’re talking about understanding your diabetes control, checking on your kidneys and liver, and looking out for other health stuff that might matter. Let’s break down the labs before starting insulin.
Key Takeaways
Before starting once-weekly insulin, doctors need to check your baseline blood sugar control, usually with an A1c test.
Kidney function is a big deal; tests like eGFR and creatinine are done because kidney problems can affect how insulin works and how it’s removed from your body.
Liver health is also evaluated with tests like ALT and AST, as the liver plays a role in processing insulin.
These initial lab results help doctors decide on the starting dose and make adjustments, especially considering any kidney or liver issues.
Understanding these labs before starting insulin is key to a safe and effective treatment plan, helping to prevent complications like low blood sugar.
Essential Blood Work Before Initiating Once-Weekly Insulin
Before you even think about starting a new insulin regimen, especially one that’s once-weekly, it’s super important to get a handle on your current health status. This isn’t just about your blood sugar; it’s a whole picture. Think of it like getting your car tuned up before a long road trip – you want to make sure everything’s running smoothly.
Understanding Baseline Glycemic Control
This is all about knowing where your diabetes management stands right now. We need to see how well your current treatment is working to keep your blood glucose levels in check. This gives us a starting point to measure progress and make sure the new insulin will be a good fit.
Hemoglobin A1c (HbA1c): This is probably the most common test. It gives us an average of your blood sugar levels over the past two to three months. A higher A1c means your blood sugar has been consistently high.
Fasting Blood Glucose: This is a snapshot of your blood sugar after you haven’t eaten for at least eight hours. It’s a good indicator of how your body is managing glucose overnight and between meals.
Random Blood Glucose: This test measures your blood sugar at any time of day, regardless of when you last ate. It can help identify spikes or dips that might not show up on other tests.
Getting these baseline numbers is key. They help your doctor figure out the best starting dose and what to aim for with the new insulin. It’s all about personalization.
Assessing Kidney Function
Your kidneys play a big role in how your body processes medications, including insulin. If your kidneys aren’t working as well as they should, it can affect how insulin works and how it’s cleared from your system. We need to check this out to make sure the insulin is used safely.
Estimated Glomerular Filtration Rate (eGFR): This is a calculation that estimates how well your kidneys are filtering waste from your blood. A lower eGFR can mean your kidneys aren’t working optimally.
Serum Creatinine: Creatinine is a waste product that healthy kidneys filter out. High levels in your blood can indicate kidney problems.
Evaluating Liver Health
Similar to your kidneys, your liver also helps process medications. Checking your liver function helps us understand if there might be any issues that could affect how the insulin is handled by your body. This is especially important when considering new diabetes treatments like once-weekly insulin icodex.
Alanine Aminotransferase (ALT): This enzyme is mainly found in the liver. Elevated levels can suggest liver inflammation or damage.
Aspartate Aminotransferase (AST): This enzyme is found in the liver, heart, muscles, and other tissues. While it can be elevated for various reasons, significant increases can point to liver issues.
Key Laboratory Tests for Insulin Therapy Readiness
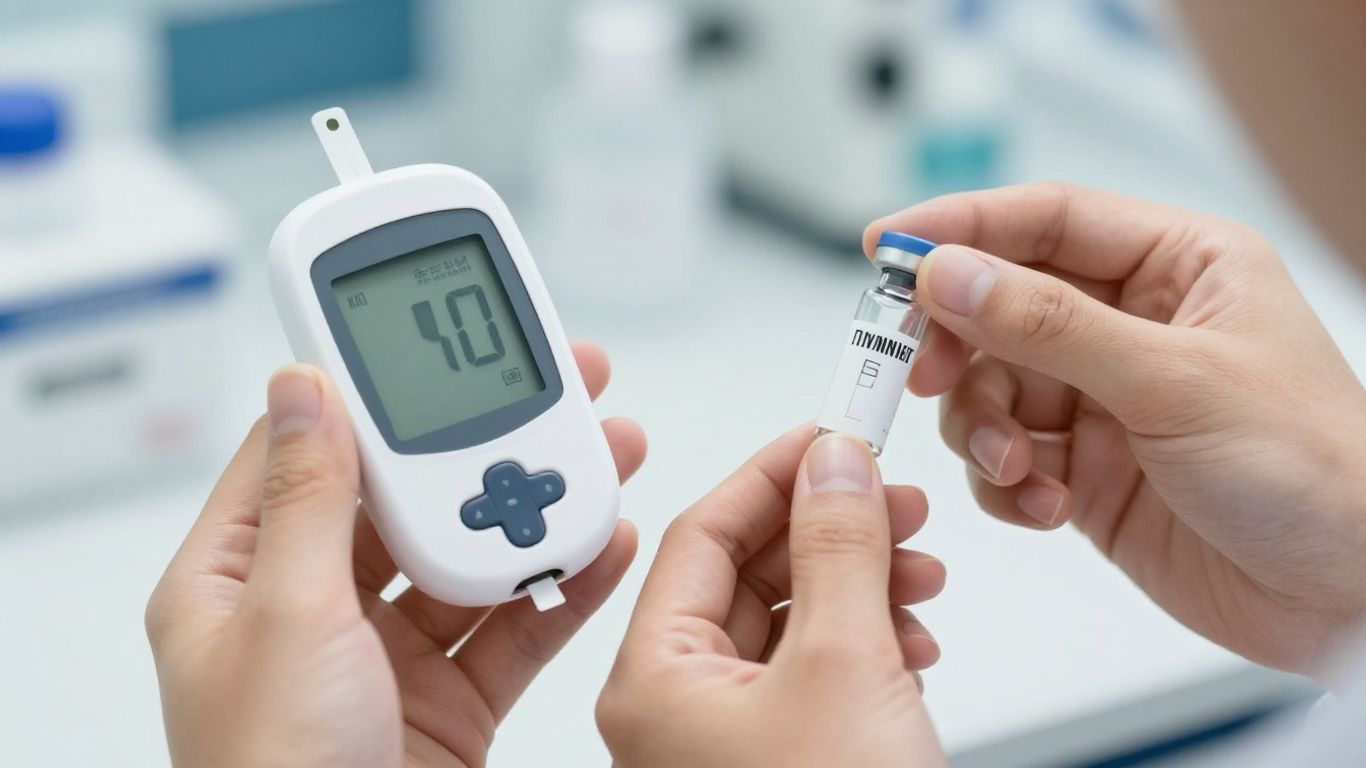
Before you even think about starting a new insulin, like the once-weekly kind, it’s smart to get a few lab tests done. These aren’t just random checks; they give your doctor a clear picture of where you stand right now. It’s all about making sure the insulin will work well for you and, just as importantly, that it’s safe to start.
Hemoglobin A1c Levels
This is probably the most common test you’ll see. Your Hemoglobin A1c, or HbA1c, gives a look at your average blood sugar levels over the past two to three months. It’s a really important number for understanding your long-term diabetes control. A higher A1c usually means your blood sugar has been running high more often. Knowing this baseline helps your doctor figure out the right starting dose for your insulin and what your goals should be.
Kidney Function Tests (eGFR and Creatinine)
Your kidneys play a big role in how your body handles medications, including insulin. Tests like estimated Glomerular Filtration Rate (eGFR) and serum creatinine check how well your kidneys are filtering waste from your blood. If your kidney function isn’t great, it can affect how insulin is processed and removed from your body. This might mean a dose adjustment is needed to prevent insulin from building up too much.
Liver Function Tests (ALT, AST)
Similar to the kidneys, your liver also helps process insulin. Tests for liver enzymes like Alanine Aminotransferase (ALT) and Aspartate Aminotransferase (AST) give clues about how your liver is doing. While insulin isn’t processed by the liver in the same way some other drugs are, significant liver issues can sometimes influence overall metabolism and how your body responds to treatment. It’s another piece of the puzzle to make sure your body is ready for insulin therapy.
Monitoring for Potential Complications
Assessing Risk of Hypoglycemia
When you start any new insulin, including once-weekly options like icodec, keeping an eye out for low blood sugar, or hypoglycemia, is super important. It’s one of the main things to watch for. While icodec is designed to be steady, there are still times when blood sugar can dip too low. This can happen more often in the first few weeks as your body adjusts, or if you change your dose, get more or less active than usual, or get sick.
Regular blood glucose monitoring is key to managing this risk. Using a continuous glucose monitor (CGM) can be really helpful, especially if you’ve had trouble noticing the signs of low blood sugar before. It gives you a clearer picture of your glucose levels throughout the day and night.
Here are some things to be aware of:
Timing: Pay extra attention to your blood sugar levels in the days after your weekly injection, particularly days 2 through 4. Some studies suggest a slightly higher chance of low blood sugar during this window.
Other Medications: If you’re taking other diabetes medications, like sulfonylureas, they can sometimes increase the risk of hypoglycemia when combined with insulin. Your doctor might adjust these other meds when you start icodec.
Recognizing Symptoms: Know the signs of low blood sugar: shakiness, sweating, confusion, rapid heartbeat, and dizziness. If you experience these, check your blood sugar and treat it promptly.
Treating hypoglycemia usually involves consuming about 15 grams of fast-acting carbohydrates, like glucose tablets or juice. If your blood sugar doesn’t improve, you might need another dose after 15 minutes. For severe episodes, your doctor might prescribe glucagon.
Evaluating Diabetes-Related Comorbidities
It’s not just about blood sugar; we also need to think about your overall health and any other conditions you might have. Diabetes can affect other parts of your body, and starting a new treatment means we need to be sure it’s a good fit for you.
Kidney Health: We already talked about checking your kidney function before starting. If your kidneys aren’t working as well as they should, it can affect how your body processes insulin, and we might need to adjust the dose. This is especially true for medications like icodec.
Liver Health: Similarly, your liver plays a role in managing blood sugar and processing medications. Any issues here could also influence how insulin works and how we dose it.
Heart Health: Conditions like heart disease are common with diabetes. While icodec has been studied alongside other common diabetes medications, it’s always good to have a general check-up on your cardiovascular health.
Other Medications: We’ll look at all the other medicines you’re taking. Some drugs can interact with insulin, either making it work less effectively or increasing the risk of side effects like hypoglycemia. It’s important to let your doctor know about everything you’re on.
Interpreting Lab Results for Insulin Dosing
So, you’ve got your lab work back, and now it’s time to figure out what it all means for your new once-weekly insulin, icodec. It’s not just about looking at the numbers; it’s about understanding how they guide your treatment. Think of it like reading a map – the labs tell us where we are and help us plan the best route forward.
Impact of Renal Impairment on Insulin
Kidneys play a big role in how your body handles insulin. If your kidneys aren’t working at full speed, it can affect how long the insulin stays in your system. This means we might need to adjust your dose. For icodec, which is a long-acting insulin, this is something we really need to pay attention to. We’ll look at your eGFR and creatinine levels to get a picture of your kidney function.
Lower eGFR: Might mean the insulin hangs around longer, potentially increasing the risk of low blood sugar.
Higher Creatinine: Also points to reduced kidney function.
Dose Adjustments: We might start with a lower dose or adjust more slowly if your kidney function is impaired.
Considerations for Hepatic Impairment
Your liver also helps process insulin. Similar to kidney issues, liver problems can change how your body uses insulin. We’ll check your liver enzymes like ALT and AST. If these are elevated, it suggests your liver might be working harder or is inflamed.
Elevated ALT/AST: Can indicate liver stress or damage.
Insulin Clearance: A less efficient liver might clear insulin more slowly.
Monitoring: We’ll likely keep a closer eye on your blood sugar levels, especially in the initial weeks.
Adjusting Insulin Based on Baseline Labs
Your starting point matters. Those initial lab results give us a baseline. If your A1c is very high, we might aim for a more noticeable initial dose to get things moving, but we have to be careful not to overdo it. Conversely, if your labs suggest a higher risk of hypoglycemia, we’ll be more conservative.
It’s a balancing act. We want to get your blood sugar into a good range without causing other problems. Your individual lab results are the key to finding that sweet spot.
Here’s a general idea of how we might think about it:
High Baseline A1c: May warrant a more robust initial dose, considering the 50% additional dose for icodec in the first week if appropriate.
Impaired Kidney/Liver Function: Suggests a more cautious approach to dosing and titration.
History of Hypoglycemia: Points towards starting with a lower dose and titrating slowly.
Insulin Resistance: Might require higher doses over time to achieve targets.
Specific Lab Considerations for Once-Weekly Insulin
When you’re looking at starting a once-weekly insulin like icodec, there are a few extra things to keep in mind, especially concerning how your body handles it. It’s not quite the same as daily insulins, so doctors want to be extra sure things are set up right.
Renal and Hepatic Adjustments for Icodec
Your kidneys and liver play a big role in how your body processes medication, and insulin is no different. For once-weekly insulin icodec, doctors will look closely at your kidney and liver function tests. If these organs aren’t working at their best, it can change how the insulin works in your body. This means the dose might need to be adjusted, or maybe even the type of insulin you use.
Kidney Function: Tests like estimated glomerular filtration rate (eGFR) and serum creatinine are key here. Lower eGFR values can mean your kidneys aren’t filtering as well, which might affect how long the insulin stays in your system.
Liver Function: Liver enzymes like ALT and AST give clues about how your liver is doing. Significant liver issues could also impact insulin metabolism.
Understanding Pharmacokinetic Properties
This just means how your body absorbs, distributes, metabolizes, and gets rid of the insulin. Because icodec is designed for once-weekly dosing, its pharmacokinetic profile is different. It’s built to release insulin slowly over the week. This slow release is great for steady blood sugar control, but it also means that if there are issues with your kidneys or liver, the insulin might hang around longer than expected.
Individualizing Treatment Plans
No two people with diabetes are exactly alike, and that’s especially true when it comes to insulin. Your doctor will take all your lab results, your lifestyle, and your specific diabetes situation into account. They’ll use this information to figure out the best starting dose and how to adjust it over time. It’s all about making sure the treatment works best for you.
Here’s a quick look at what might be considered:
Baseline Labs: Your starting A1c, kidney function, and liver function tests are the foundation.
Other Medications: What else are you taking? Some drugs can interact with insulin or affect your blood sugar.
Personal Health History: Any past issues with hypoglycemia or other diabetes complications are important.
It’s really important to have an open chat with your healthcare provider about your lab results. They can explain what everything means in the context of starting a new insulin regimen and help you feel confident about the plan moving forward.
Wrapping Up
So, before you start that once-weekly insulin, remember to chat with your doctor about getting those key lab tests done. It’s all about making sure this new treatment works well for you and stays safe. Checking things like your kidney and liver function, and keeping an eye on your blood sugar levels, helps your doctor figure out the best starting dose and how to adjust it. It’s a team effort, really, to get your diabetes management on the right track with this new option.
Frequently Asked Questions
Why do I need lab tests before starting a once-weekly insulin shot?
Before you start a new medicine like once-weekly insulin, doctors want to check a few things about your body. This helps them make sure the insulin will be safe and work well for you. They check your blood sugar levels to see how well your diabetes is controlled now. They also check your kidneys and liver to make sure these organs are working okay, as they help your body process the medicine.
What is Hemoglobin A1c, and why is it important?
Hemoglobin A1c, or A1c for short, is a blood test that shows your average blood sugar level over the past 2-3 months. It’s like a report card for your diabetes control. A high A1c means your blood sugar has been high on average, and a lower A1c means it’s been more controlled. Your doctor will look at your A1c to decide if once-weekly insulin is the right choice and how to start it.
How do kidney and liver tests affect my insulin treatment?
Your kidneys and liver help get rid of medicines from your body. If your kidneys or liver aren’t working as well as they should, the insulin might stay in your body longer. This means your doctor might need to adjust the dose of your once-weekly insulin to prevent it from causing problems, like blood sugar dropping too low.
What is hypoglycemia, and how do lab tests help prevent it?
Hypoglycemia means your blood sugar is too low. It can happen with insulin. Lab tests help your doctor understand your usual blood sugar levels and how your body handles medicine. This information helps them choose a starting dose for your insulin that’s less likely to cause your blood sugar to drop too low, making your treatment safer.
Are there special things to consider for once-weekly insulin compared to daily insulin?
Yes, once-weekly insulin, like insulin icodec, is designed to last longer in your body. This means doctors carefully check your kidney and liver function because these organs play a big role in how your body uses this longer-acting insulin. They want to make sure it’s used safely and effectively for you.
Can other medicines affect how my once-weekly insulin works?
Absolutely. Some other medicines you might be taking for diabetes or other health issues can change how much insulin your body needs. For example, certain diabetes pills can either make your body need more insulin or less. Your doctor will look at all your medications to make sure they work well together with your new once-weekly insulin and to lower the chance of problems.
Need A Lab Test?
We can help.
HOW TO BOOK
01. Choose From Our Various Tests
Choose the right test(s) from our comprehensive selection to meet your specific health needs.
02. Prepare Your Infomation
Gather your name, birth date, contact info & specific tests.
03. Book In
Call us up and we will get you scheduled for your lab draw or book through our virtual calendar by clicking here.
